After several examinations and many consultations with neurologists, physical medicine specialists and neurosurgeons, the diagnosis was made: Absolute vertebral stenosis C3/C4; neuroforaminal stenosis C5–C7.
With such a clear diagnosis, no time could be wasted; only surgeries can protect the spinal cord from irreversible damage. Even a minor accident (for example a fall) could cause severe damage to the spinal cord in that area. The result can be a high-level paraplegia.
The five-day preparation then began, involving daily washing of the body and hair with a special soap and the use of a cleansing nasal ointment. In addition, the bed linen and clothes had to be changed daily.
On the morning of my surgery, many thoughts went through my head: Have I packed everything? My health insurance card and the CDs with my test results are packed. My hygiene items and clothes are in my suitcase. I’m still allowed to lift it now. Starting next week, I’ll only be allowed to carry 2 kilograms. How is that even possible? My cell phone and charger are within easy reach. Who do I have to share a room with? I hope everything goes well. Maybe one operation will be enough. All these thoughts are probably shared by the patients we care for in hospital. Young people, especially those staying in the hospital for extended periods, need roommates they get along with. Fears, distress and worries are best discussed with trusted individuals.
Soon after, I received a very warm welcome at the neurosurgery ward. The nursing team was already waiting and accompanied me to my two-bed hospital room. I quickly filled out some forms and carefully put my clothes in the wardrobe. Then lunch arrived. The afternoon passed with doctors’ visits, watching television, reading the newspaper, and visiting from friends and family. Around 10 p.m., a surgeon came and explained the surgery to me and marked an X on my neck. Then came my washing ritual. I was first on the surgery list.
I was woken up around 5:30 a.m., and then the daily washing ritual began. Afterward, I lay down in a sterilely prepared bed in the hallway. My surgeon greeted me, and passing staff wished me well. Finally, I was taken down to the surgery room waiting area. Shortly afterward, I was lying on the surgery table.
Around 6 p.m., I woke up in my room. I was tired but pain-free. The venous pump was working hard. The nursing staff regularly checked the infusion and the catheter. That’s how the first night passed.
In the morning, I was given a small breakfast. After my temperature was taken, I was allowed to get up, accompanied by someone. Ihhh! That was awful. My circulation completely collapsed. I was quickly back in bed with my footrest raised and a new infusion drip. The second day wasn’t much better. Luckily, the nursing and medical team were always there to help. Service assistants and cleaning staff also did their jobs in the room. They always had a few encouraging words for us patients. I felt a little better on the third day, but on the fourth day, my blood pressure was very low again, and even the shortest walk was difficult. Nevertheless, I felt safe in the hospital. Almost all patients in the hospital have these experiences.
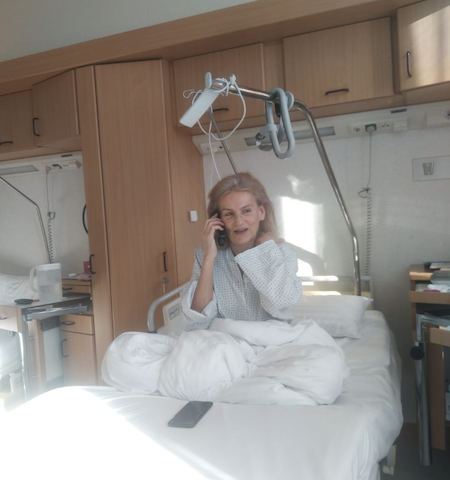
The phone was a wonderful lifeline to the outside world
Children and teenagers who don’t yet know how to cope with such situations often react in their despair with defensiveness or withdrawal in class. After over 30 years of service as a hospital teacher, I know how burdened children are in the hospital. I constantly try to understand their feelings and worries and to address their individual needs. My own hospital stay has made me even more sensitive to their needs. Difficulty concentrating, easy distractibility, forgetfulness, as well as irritability, impulsiveness, restlessness, and daydreaming often result from their helplessness. Currently, I’m paying more attention to helping them overcome these painful feelings of powerlessness. Dedicated space and time, along with small, manageable cognitive tasks, are intended to help them experience success. Health comes first, followed by the pressure-free achievement that is a part of life.
Two days later, after the discharge interview, receiving the discharge letter and confirmation of stay, I was discharged and sent home, and rehabilitation began.
Brigitte Gruber (from Austria)
Email address: brigittegruber.dr.mag@web.de